Threats to ambulance services increase rural health insecurity
Dearth of volunteers, paramedics, funding creates uncertainty
BISMARCK, N.D. – A motorcycle crash on a deserted road. A cardiac arrest at a far flung farm in a rural county. A farming equipment accident. A pregnant woman goes into unexpected labor at a small hamlet away from population centers.
When these emergency medical scenarios happen in rural communities across North Dakota, local volunteer first responders are often the first on the scene, the first to provide medical attention, and the first to get patients to a hospital.
Many of these services are in trouble, however.
A lack of volunteers and younger staff willing to commit the time and energy needed to the profession, the challenge of recruiting and retaining paramedics, and a constant uncertainty about funding at a time of increasing costs threatens the sustainability of many services.
Legislation was recently approved for mandating and funding ambulance districts, but it is too early to understand how much of an impact the rules will have.
Andrew Berkey, operations manager of Jamestown Area Ambulance – Ringdahl EMS, said he’s been short-staffed for at least the past six months. Costs have also continued to skyrocket. That’s led to increased workload both for himself and his remaining staff and threatens the operability of the service.
“We’re in a really scary place,” Berkey said.
Staffing plus equipment costs for a service of two people operating an ambulance available 24 hours a day, seven days a week ranges from between $700,000 to around $1 million annually, according to a study led by Yvonne Jonk at the University of Southern Maine.
“It’s very hard to pay paramedics and EMTs what they’re worth and keep your doors open,” Berkey said.
Costs for a new ambulance have also doubled in the past several years from around $100,000 to over $200,000, Berkey said.
Ambulance deserts
Jonk, who also recently released a study looking at what are called “ambulance deserts” – or areas where it takes 25 minutes or longer for an ambulance to arrive on scene – said North Dakota has one of the lowest rates for ambulances per square mile, but one of the highest rates of ambulances per 100,000 residents.
“The problem is that they’re so danged spread out that it’s hard to provide adequate coverage in a state that’s so sparsely populated,” Jonk said.
All counties across the state have at least one area that would be considered an “ambulance desert,” according to the study. North Dakota also joins other Western states of Idaho, Nevada, New Mexico, South Dakota, Utah and Wyoming as states where there are fewer than three ambulances per 1,000 square miles.
Jonk said the “low volume, high cost” operations predominately in rural areas are under threat due to increasing costs. She said her study found the breakeven amount for a response can range from $1,000 to $41,000.
“You know, it's like, there's no way they're going to be reimbursed $41,000 to bring somebody to the hospital and they're only reimbursed if they bring somebody to the hospital,” Jonk said.
Jonk is working on another study that looks at the numbers of paramedics available in rural areas and survival rates related to cardiac arrest, and expects those numbers are also going to show a widespread shortage.
“If you’re having a heart attack you want a paramedic, as opposed to an EMT, because they all know what to do,” Jonk said. “Survival rates will definitely be higher amongst those services that have a paramedic on board.”
Chasity Dixon, who works as a paramedic with the Community Ambulance Service Rolla, said that rural services that don’t have paramedics lose out on revenue generated from transferring patients between hospitals.
“It helps fix staffing problems and helps with revenue so you can pay people to be available,” Dixon said of the need of having a paramedic on staff.
Essential services
While most would consider ambulance services as essential for community health, they are not staffed and funded like other services - police, many fire departments, garbage collection, road plowing and maintenance. They can sometimes go a week without a call. Other weeks they’ll have calls daily.
“Ambulance services are not considered essential services,” Dixon said. “Even when it’s the cops that are down, it is us that are coming to take care of them so you’d think that we’d be essential services, but we’re not.”
James Owen, president and an EMT at Gackle Ambulance Service, said the service has been running with a skeleton crew for years and is in constant need for EMTs and drivers, but accessing that workforce has been problematic.
“Long term we need to recruit and get younger individuals involved in serving and volunteering,” Owen said.
Cory Schwarz, vice president of the Gackle service, said there appears to be an erosion of values and community service among the younger generation that remains in the area.
“I think the biggest issue with trying to get younger people is they're just not interested,” Schwarz said. “They think, well, somebody else will take care of it. Somebody else will do it. So I don't have to worry about it.”
Lindsey Narloch, a project manager at the North Dakota Emergency Medical Services Association (NDEMSA), said that while rural ambulance services have long been built on the backs of volunteers, this has been changing as society changes.
“Now most households have two people working. Farms have become bigger, leaving fewer people. Many work in other cities and live in rural or frontier cities so there may be no one to cover during the work week hours, where before an employer in town would let the EMT leave,” she said.
Other ambulance crew members also mentioned challenges from their regular employers not allowing as much flexibility as they had in the past as well as petty local politics that disrupts continuity of services.
Promise of 1365
Potential exists, however, for beefing up rural ambulance services and making them more essential in the state.
Currently, rural ambulance services are compensated through medical insurance claims, some mill levy proceeds and by fundraising and donations.
House Bill 1365, passed by legislators earlier this year, will require areas to form rural ambulance districts and give them the ability to levy a local tax after approval from voters to help support that service, practitioners say.
Adam Parker, advocacy chair for NDEMSA, said the measure could dramatically change the landscape for rural emergency medical services by mandating the formation of ambulance districts.
“These districts will be able to levy taxes to support the districts, if approved by the local voters, to support a sustainable EMS program for the district,” Parker said. “There is a lot of work to be done over the next two years to establish districts across the state and solidify an infrastructure that will serve North Dakotans long into the future.”
Sean Roed, a paramedic and director of operations at the Lake Region Ambulance Service, said his team has already started working on formulating a tax district board. He said he hopes the bill can make ambulance services in the state “more of a profession” and an essential service.
“So by June of next year we’ll be on the ballot, and then, if things are voted right and in our favor, by January 2025 we’ll have additional funding.”
Filling training gaps
Another aspect of rural ambulance services that often takes additional time and energy from volunteers and essential workers is the need to constantly refresh skills and meet certification requirements.
This was something that didn’t exist a few decades ago when most ambulance services were tasked simply with transferring people to a medical facility without rendering life-saving aid.
Not only is some of the training time consuming, rural ambulance workers often have to travel distances to attend classes if they’re not available online.
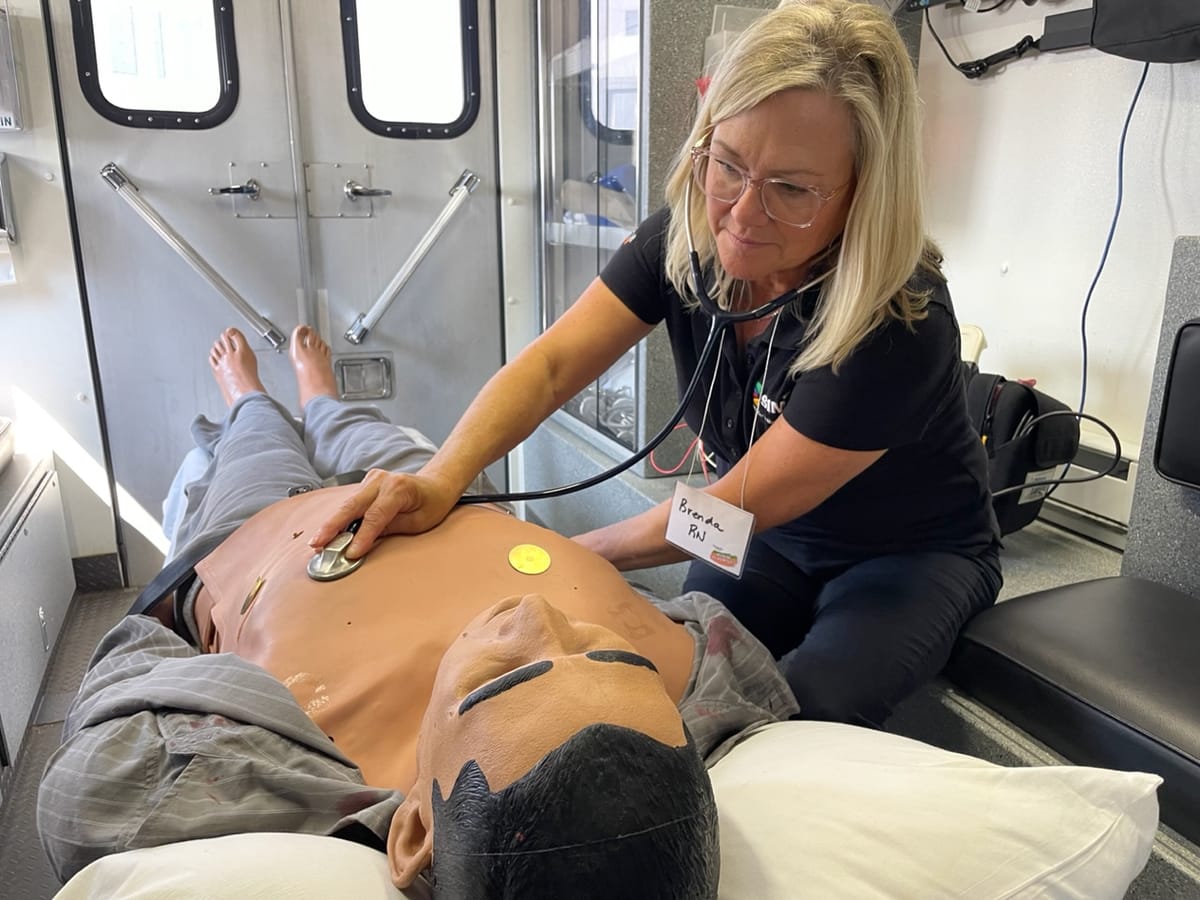
One service that has helped fill this gap is Simulation in Motion or SIM-ND mobile labs, administered through a project at the University of North Dakota. Mobile labs provide free certification training on lifelike mannequins transported throughout the state to critical access hospitals, rural ambulance services and others such as law enforcement.
These mobile labs provide crying, breathing, talking mannequins ranging from adults, to children and infants, as well as soon-to-be mothers on the verge of labor.
“This was based on work that we did that showed needs such as taking care of heart attack patients, precipitous deliveries when they usually don’t do many deliveries, farm accidents and that kind of thing,” said Jon Allen, director of the UND SMHS Sim Center & SIM-ND Mobile Simulation.
Jessi Nicola, administrator of the program, said a primary goal of the program is to provide free training to medical personnel where they are due to a variety of challenges faced in rural areas.
“A lot of those places don’t have a lot of people, so you can’t really give up your only ambulance driver or your only EMT in that area just to go to training,” Nicola said. “So we try to come to them and give them up to date training with staff who are experienced.”
The North Dakota News Cooperative is a nonprofit news organization providing reliable and independent reporting on issues and events that impact the lives of North Dakotans. The organization increases the public’s access to quality journalism and advances news literacy across the state. For more information about NDNC or to make a charitable contribution, please visit newscoopnd.org. Send comments, suggestions or tips to michael@newscoopnd.org. Follow us on Twitter: https://twitter.com/NDNewsCoop.



